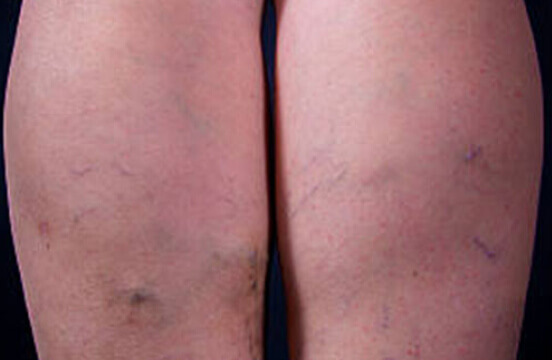
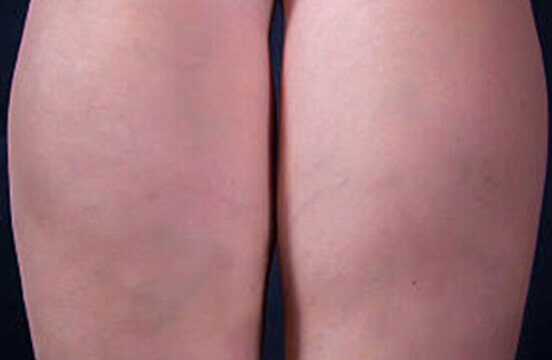
Our Michigan Vein Doctor Explains Deep Vein Thrombosis
Imagine experiencing an intense pain in your calf — one that only worsens with time and leaves you feeling restless at night. After putting off medical attention for too long, you could suddenly find yourself facing a life-threatening condition. This alarming reality can quickly become true for individuals suffering from deep vein thrombosis (DVT).
Untreated DVT has the potential to progress into significant health issues or even prove fatal. Our Michigan vein doctor will dive into the causes, symptoms, and treatment options of this vascular condition, ensuring your understanding of DVT goes beyond its ominous nature and equip you with the knowledge you may need.
Understanding Deep Vein Thrombosis
Deep vein thrombosis (DVT) is a potentially dangerous condition that develops when a blood clot forms in deep veins, usually in the legs. The formation of blood clots in veins is a normal response to injury or bleeding, and it helps to stop bleeding by blocking off the damaged veins. However, if blood clots form when they’re not needed, they can restrict blood flow and cause serious complications.
DVT is often unrecognized and diagnosed too late as its symptoms can be nonspecific and similar to other conditions, like leg cramps or swelling. For example, heavy exercise can make the legs tired and lead to swelling — which might be confused with DVT symptoms, since both conditions share similarities. DVT may also exist without presenting any obvious warning signs for extended periods before becoming life-threatening.
Not everyone who develops DVT experiences serious complications, and this condition can often resolve itself without medical intervention. Nevertheless, the risk of complications associated with untreated DVT is concerning — such as pulmonary embolism (PE), stroke, or death — all results that can be avoided with proper diagnosis and management.
Causes and Risk Factors
DVT can stem from a single factor or a combination of several. The most common causes include:
- Injury
- Long Periods of Immobility
- Surgery
- Cancer
- Other Diseases
- Hereditary Disorders
- Pregnancy-Related Situations
Various risk factors can contribute to the development of DVT.
- Being inactive for lengthy periods
- Sitting for extended periods
- When sitting still for too long without contraction
- Individuals who are over 40 years old
- Obesity
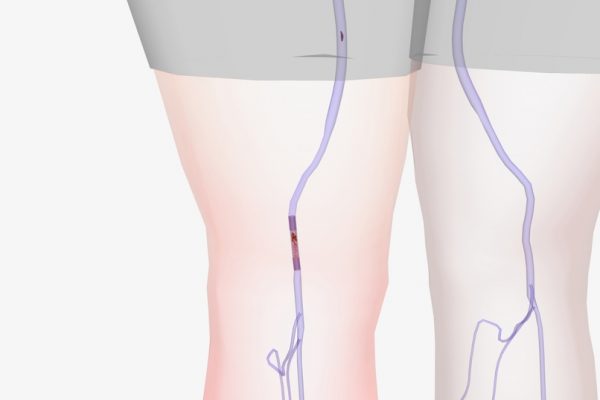
Symptoms and Complications
Deep vein thrombosis may not always present noticeable symptoms, but when they do, they can be similar to those of other conditions. Pain and swelling are the most common indicators of DVT, but other potential symptoms include:
- Warmth or redness in the affected area
- Skin discoloration, typically blue or purple
- Tenderness in the affected area
- Enlarged veins on the surface
These symptoms may appear suddenly or gradually and are often mild at first. However, if left untreated, DVT can cause serious complications such as pulmonary embolism (PE), which can be life-threatening.
In addition to PE, untreated DVT can lead to other serious complications, such as:
- Post-Thrombotic Syndrome: A condition that causes long-term leg pain, swelling, and skin ulcers.
- Chronic Venous Insufficiency: Condition where damaged veins disrupt blood flow, leading to varicose veins, skin changes, or ulcerations.
- Pulmonary Hypertension: A rare condition where high blood pressure damages arteries in the lungs, leading to heart failure.
While some patients with deep vein thrombosis may not experience significant pain or swelling, this doesn’t necessarily mean that there’s no need for treatment. Any signs or symptoms should be reported to a qualified medical provider immediately. Even mild DVT cases have the potential to develop into more severe complications.
Ignoring minor problems like leg achiness, soreness, calf pain, or puffiness may lead to more significant health concerns in the long term. If you’re experiencing symptoms of DVT, contact our Michigan vein doctor today for an appointment.
Detecting Pulmonary Embolism
Pulmonary embolism (PE) is a potentially life-threatening condition that occurs when a DVT blood clot dislodges from the vein wall and travels through the bloodstream until it lodges in the lungs. Early detection of PE is essential because it requires expert care and management at medical facilities specializing in pulmonary arterial hypertension.
Symptoms of PE can include:
- Sudden shortness of breath
- Chest pain
- Rapid pulse
- Lightheadedness or dizziness
- Unexplained cough that may include coughing up blood
PE’s severe symptoms necessitate immediate medical attention and potentially emergency services to ensure that no further damage or risk occurs.
Individuals with underlying conditions such as cancer, sickle cell disease, heart failure, or autoimmune diseases may be at greater risk of developing PE than those without any known predisposing factors. It’s even more critical to remain vigilant about minimizing risks and seeking prompt and appropriate treatment following the diagnosis of DVT.
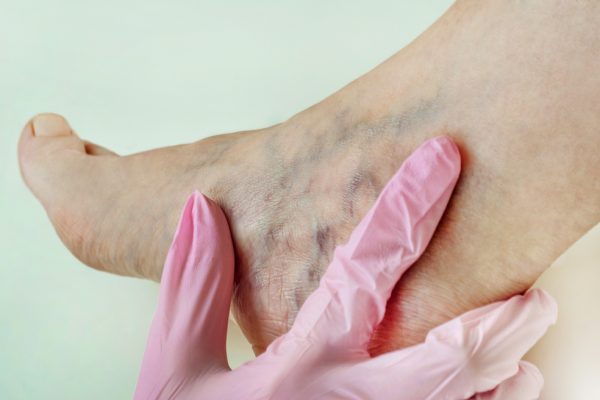
Diagnosing Deep Vein Thrombosis
Diagnosing deep vein thrombosis can be challenging because the symptoms may not always be noticeable or only occur in mild forms. It’s crucial to get a proper diagnosis as soon as possible to avoid further complications. Doctors usually rely on several factors to diagnose DVT, including medical history, physical exams, blood tests, and imaging tests.
If you have a family history of DVT or other clotting conditions, your doctor will want to know. They’ll also inquire about any medications you’re taking and lifestyle factors such as how much you exercise, whether you smoke, and if you travel frequently.
Physical exams are also essential in diagnosing DVT. The doctor may examine your legs for swelling, tenderness, warmth, or redness that might indicate the presence of a clot. They’ll also check your pulse rate and blood pressure to see if they’re elevated or unusually low.
Blood tests don’t always provide definitive proof of DVT’s existence. However, these tests can still be useful as they help identify signs of inflammation that might indicate that there’s a clotting issue. Imaging tests are also incredibly helpful for identifying the location and severity of blood clots.
Imaging Tests and Procedures
Once vein doctors suspect that you might have a blood clot, they’ll recommend further tests and procedures to confirm the diagnosis and evaluate the extent and location of the clot.
One commonly used imaging test for diagnosing DVT is venous ultrasound (US). During this test, high-frequency sound waves create images showing blood flow through veins in the legs or other parts of your body. The test is noninvasive, painless, and takes only 30 to 40 minutes to complete.
Magnetic resonance venography (MRV) may be necessary if there’s uncertainty about the diagnosis after an ultrasound scan. This imaging technique provides a detailed image of veins in the legs and pelvis using a powerful magnetic field. During the procedure, you lie down on a table that slides inside the MRI scanner.
If your doctor suspects that you might have a pulmonary embolism, they may recommend a computerized tomography pulmonary angiography (CTPA). A CTPA is a type of CT scan that focuses on blood vessels in the lungs. CTPA uses contrast material or dye injected into a vein in your arm to create detailed images of your lungs’ blood vessels. It highlights the areas with clots so doctors can assess the severity of the PE involved.

Treatment Strategies
There are various vein treatment options available.
Blood Thinners
In most cases, blood thinners such as warfarin and heparin can prevent further clotting and allow the body’s natural healing process to occur. Blood thinners work by preventing the formation of new clots while allowing the existing ones to dissolve gradually. Depending on the severity of the clot, these medications may need to be taken for several weeks or months.
Compression stockings
Compression stockings are an aspect of DVT treatment that helps prevent post-thrombotic syndrome (PTS). PTS is a long-term complication caused by poorly healed vein damage after a blood clot has been resolved. Compression stockings are tight-fitting garments designed to exert pressure on the legs, ankles, and feet. This pressure helps improve blood flow and reduces swelling in the legs.
Surgery
Surgery is relatively rare in DVT cases but may be recommended if there’s significant damage to your veins or if there’s a large clot that needs urgent removal. Thrombectomy or catheter-directed thrombolysis are two surgical procedures commonly used in removing DVT blood clots.
Medications and Lifestyle Changes
Medications are often recommended as an initial therapy for treating DVT. However, lifestyle changes can help increase effectiveness and prevent future recurrences of DVT.
- Exercise is an effective way to improve circulation and reduce the risk of DVT. Regular physical activity can help strengthen the calf muscles, which push blood back up to the heart. Even simple activities like walking, cycling, or swimming can help.
- Maintaining a healthy weight is another significant lifestyle change that can reduce the risk of DVT. Being overweight or obese increases the pressure on your legs and veins, leading to poor blood flow and increasing your chances of developing DVT. Excess weight puts extra pressure on the veins and restricts blood flow.
- Quitting smoking is also highly recommended for reducing the risk of DVT. Smoking constricts your blood vessels, reduces oxygen supply, and creates a higher risk of damage to your blood vessels.
Frequently Asked Questions
The main causes of deep vein thrombosis (DVT) can fall into three categories:
- Temporary and reversible factors
- Inherited conditions
- Chronic medical conditions
Temporary factors include prolonged immobility, such as during long flights or bed rest after surgery, while inherited conditions like Factor V Leiden mutation increase the risk of clotting. Chronic medical conditions like cancer, heart disease, and obesity may also contribute to DVT risk.
Deep vein thrombosis commonly develops in the lower leg, often remaining undetected as it naturally resolves over time. However, it can manifest symptoms like pain and swelling. If an individual is diagnosed with DVT, prompt treatment becomes necessary to prevent severe complications like pulmonary embolism.
Yes, walking can be beneficial for individuals with deep vein thrombosis (DVT). It’s generally recommended as part of the treatment and management plan for DVT. Walking helps improve blood circulation, which can prevent blood from pooling in the veins and reduce the risk of blood clots. However, consult with a healthcare professional before starting or modifying any exercise regimen, as they can provide personalized advice based on the individual’s specific condition and medical history.
Contact Our Michigan Vein Doctor for an Appointment!
At Suburban Vein Center, our Michigan vein doctor will work with you to ensure you obtain the right diagnosis and most effective treatment. If you suspect you may have DVT, contact one of our four Michigan vein clinics today. Schedule your appointment today by calling (248) 480-0368.
With offices located in Troy, Taylor, Rochester, and Detroit, we’re here to get you the care you need.